Max Whooley MS 2, Kayla Aikins MS 3, Brian Gilmer, MD
Distal femoral osteotomy
Distal femoral osteotomy (DFO) is a joint-preserving surgical procedure used to correct improper alignment of the femur and tibia in a condition known as valgus deformity. Valgus deformity causes a “knock-knee” appearance and places increased load on the lateral compartment of the knee joint. Varus, or “bow-legged”, deformity causes the opposite problem, placing increased load on the medial compartment.6 DFO is typically performed in patients with isolated osteoarthritis of the lateral compartment of the knee due to valgus deformity, in order to reduce excessive load in that area and avoid the need for a joint replacement procedure in relatively young, active patients.4,7
Indications & Contraindications
A valgus tibiofemoral angle of 5°-8° is considered physiologically normal.4 Valgus knee deformity beyond this point is associated with excessive compressive forces on the lateral compartment of the knee. Overtime, this may progressively damage the cartilage of the knee joint leading to osteoarthritis in this compartment. A tibiofemoral angle greater than 12° is considered severe valgus deformity.1 The severity of valgus deformity correlates with the extent of cartilaginous breakdown.6 Lower limb malalignment has the potential to cause deviations in gait along with ligament imbalance in the knee.1
DFO is indicated in patients with:
- Valgus deformity (tibiofemoral angle >8°)1
- Knee pain7
- Isolated mild to moderate lateral compartment osteoarthritis5,7
- Lateral condyle cartilage lesions5
- Lateral meniscus transplants5
- Non-operative treatment failure7
DFO is contraindicated in patients with:
- Severe medial compartment or tricompartmental osteoarthritis3
- Valgus deformity >20° [4]
- Severe articular damage (Ahlbäck Grade III or higher)4
- Poor knee ROM (<120° of flexion)4
- Inflammatory arthritis3,4 such as rheumatoid arthritis2
- Severe osteoporosis3
- Severe ligament instability4
- Tibial subluxation >1 cm [4]
Relative contraindications include severe patellofemoral arthritis, elevated BMI, nicotine use, and age >55. [3,5]
Causes of Valgus Knee Deformity
- Trauma1,2
- Inflammatory disorders4
- Metabolic disease such as renal osteodystrophy1,2
- Complication of lateral meniscectomy1
- Other disorders of growth plate morphology1
Diagnosis & Pre-Operative Planning
Using lower limb x-rays, a weight-bearing line is drawn from the center of the femoral head to the center of the talus. A diagnosis of valgus deformity is confirmed if this line runs through the lateral compartment rather than the center of the knee. Lines must then be drawn from the centers of the femoral head and talus to the center of the intercondylar notch, in order to calculate the precise angle of correction necessary to restore normal anatomic alignment and to select an appropriate wedge size.5 If suspected during preoperative evaluation, articular, meniscal, or ligament pathology may be evaluated by MRI and further assessed by diagnostic arthroscopy.3,5 This will help determine if concomitant procedures such as lateral femoral condyle osteochondral allograft transplantation3 or ligament reconstruction4 may need to be performed prior to osteotomy.
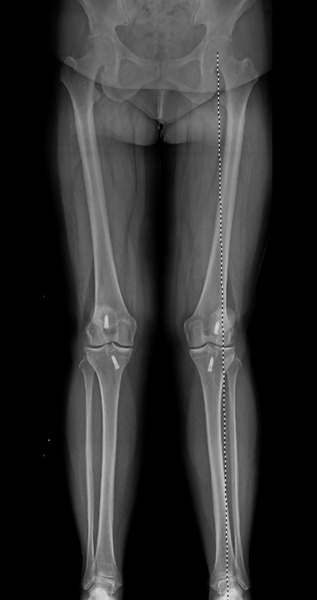 Figure 1
Figure 1
In this x-ray the patient is standing up and the weight moves from the hip to the ankle. In this case, the deformity is valgus or ‘knock-kneed’ and too much pressure is passing through the outside of the knee joint. Incidentally the patient has had ACL surgery on both knees in the past and the metal screws can be seen as white objects on each side of the knee. The patient is starting to develop arthritis in the outside portions of the knee (lateral).
Indications
Coronal DFO is indicated for patients experiencing abnormal alignments of the bones that involve the knee joint. The procedure should be considered in active patients less than 65 years old (and typically much younger than this since partial knee replacement may be a better option for older patients) who are affected by osteoarthritis or other conditions that result in misalignment of the knee3. Activity level, lifestyle, and general health should be considered prior to surgery. In addition, a variety of medical conditions can result in deformities that may benefit from coronal DFO:
- Isolated arthritis along the lateral compartment of the knee. Arthritis can result from previous trauma, or from genetic predisposition. Surgery allows these patients to shift their weight from the lateral surface of the knee to the medial surface where normal cartilage is located.
- Chronic medial collateral ligament (MCL) tear in valgus alignment requires surgical correction. Otherwise, there is an increased risk that the MCL tear will progress.
- Valgus malalignment of the knee causes pain and discomfort, while increasing risk of lateral meniscus and chondral (cartilage) injury, as well as eventually arthritis (OA). Mechanical realignment should be considered.
Causes
The cause of valgus malalignment is not known, in some cases this is simply genetic, however, to consider realignment there has often been prior trauma or surgery that results in the malalignment being severe enough to consider intervention.
Surgical Procedure
The two main technical options for a distal femoral osteotomy include a medial closing wedge DFO and a lateral opening wedge DFO. Both techniques effectively produce a varus correction to the valgus deformity to restore normal physiologic alignment of the lower limb. The currently available literature supports positive outcomes in both procedures, and the superiority of either surgical option has not been determined. Dr. Gilmer prefers a lateral approach as it is more familiar, potentially safer, and a bit easier because the other leg is not in the way while operating from the lateral side. We will discuss both techniques below, but again, Dr. Gilmer prefers a lateral opening wedge.
The advantages of lateral opening wedge DFO over medial closing wedge DFO include:
- More precise intraoperative correction3,4
- Easier surgical approach3 & execution1
- Better lateral compartment access for concomitant procedures5
- More suitable for medium to large deformities7
- Better tension & mechanical advantage4
- Less plate intolerance4
The disadvantages of lateral opening wedge DFO over medial closing wedge DFO include:
- Bone grafting necessary5
- Increased risk of non-union3
- Less suitable for small deformities7
- No immediate post-operative loading5
- Later mobilization5 & longer healing time7
Both surgeries are performed under general anesthesia and require the patient in a supine position in full knee extension. The operative leg may need to be raised on a foam ramp or manipulated intraoperatively to allow for optimal views of fluoroscopic imaging and to avoid iatrogenic injury.3,5
Medial closing wedge: With the knee extended, a 10 cm incision is made from the medial epicondyle to the joint line. This incision continues through the subcutaneous tissue through the vastus medialis fascia. The vastus medialis muscle is lifted anteriorly from the intermuscular septum to expose the medial distal femur. All vasculature in this area must be carefully cauterized. A locking femoral plate is placed on the distal femoral cortex in order to mark the osteotomy site at the metaphyseal-diaphyseal junction. Retractors are used to hold the vastus muscles and neurovasculature away from the osteotomy site. Two guide pins are then inserted through the medial cortex at the precise angle of correction calculated preoperatively to form an apex about 5mm medial to the lateral cortex. An oscillating saw is used to cut along the guide pins, sparing the lateral cortex. Irrigation must be used to prevent thermal necrosis of bone. Using fluoroscopic guidance, the surgeon will resect the bone wedge and manually compress the bone to close the osteotomy. Once a neutral weight-bearing axis through the center of the knee joint has been confirmed, the locking plate is placed onto the medial distal femoral cortex to traverse the osteotomy site and is temporarily secured with two pins, each inserted into a distal and proximal hole. Multiple locking screws are inserted into the distal plate holes. The osteotomy must be further compressed using a 4.5 mm cortical screw inserted at the most distal hole with a slightly proximal and lateral trajectory. Finally, multiple locking screws are inserted into the proximal plate holes and the vastus medialis muscle is sutured back to the intermuscular septum prior to wound closure.5
Lateral opening wedge: A 12-15 cm incision is made over the lateral distal femur. The iliotibial band is split and the vastus lateralis muscle is lifted anteriorly from the intermuscular septum to expose the femoral shaft. Branches of the deep femoral artery (profunda femoris) must be carefully cauterized at this point. Next, a guide pin is placed approximately 2-6 cm proximal to the lateral epicondyle, aimed with a slightly distal trajectory through the metaphyseal-diaphyseal junction towards the medial epicondyle. The anticipated osteotomy site is marked on the cortex and the knee is then flexed to decrease tension and reduce risk of neurovascular injury. An oscillating saw initiates the cut along the guide pin into the bone, which is completed with osteotome instruments, sparing the medial cortex of the femur. A jack opener is used to open a wedge within the bone, and a bone graft is inserted into the osteotomy site.3 Multiple bone graft choices may be utilized during open-wedge procedures, including allograft, calcium phosphate cement, cortical iliac crest autograft, and tricortical iliac crest allograft. An optimal graft choice is unclear based on the available literature.1 Fluoroscopy is used to confirm the planned degree of correction has been properly executed and has created a neutral mechanical alignment. A locking plate can then be placed onto the lateral distal femoral cortex to traverse the osteotomy site. Multiple locking screws are inserted through the distal plate holes, followed by a non-locking compression screw to temporarily hold the bone graft in place. Finally, more locking screws are inserted into the proximal holes of the plate to adequately secure the correction.3
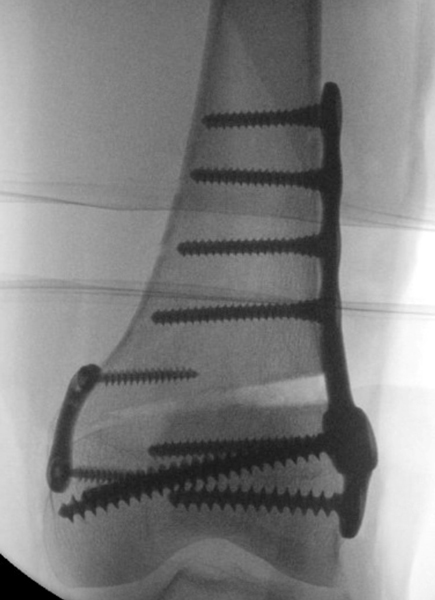 Figure 2
Figure 2
Here is one image taken during surgery showing the gap created on the outside of the femur bone. Dr. Gilmer typically performs a lateral opening wedge osteotomy and so this is the technique shown here. The small plate on the medial (inside) part of the knee is there to relieve stress at the hinge point of the osteotomy and reduce the risk of fracture.
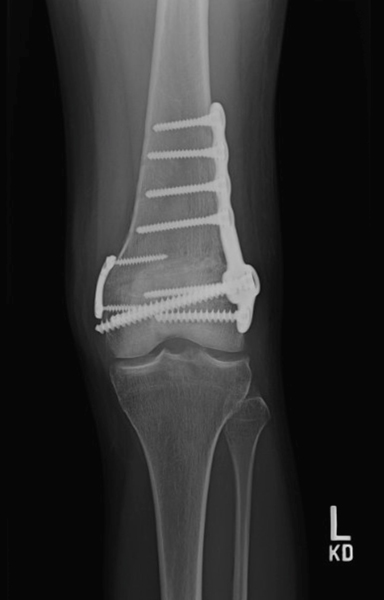 Figure 3
Figure 3
This xrays shows one plate and screw combination used for holding the osteotomy. You can see that in these images the triangular wedge is barely visible – the osteotomy has healed and filled with the patient’s own bone.
The medial closing wedge DFO is performed in a similar manner, except it is performed on the medial side of the femur, and the opening is closed by bringing the cut ends of bones together, thus altering bone alignment4.
Risks and Complications
This procedure is challenging and has a relatively high complication rate ranging from 5-63%. Fortunately, many of these complications are not serious but may require additional surgery. All surgical interventions have inherent risks. The most frequently reported complication of a DFO is a hardware-related issue such as plate discomfort, prominence, or irritation.1 Other possible risks and complications include:
- Knee stiffness1,4
- Post-operative pain1,4
- Malcorrection3
- Nonunion or delayed union (joining) of bone4
- Infection4
- Neurovascular Injury3
- Fixation failure4
- Hematoma1
- Femur fracture1
- Intra-articular fracture3
- Arthrofibrosis/Contracture3
- Deep vein thrombosis3
- Pulmonary embolism1
Post-operative care
Rehabilitation begins immediately following the surgery. Patients are placed on a deep vein thrombosis prophylaxis agent to prevent blood clots. The surgical site is dressed with sterile cotton and a bandage. The leg is stabilized in an immobilizer that holds it in full extension, and the patient must refrain from walking for 6 weeks with minimal weight-bearing. During that time, specific exercises are allowed to maintain range of motion. After 3 months, radiographs are taken to determine whether or not the deformity was appropriately corrected5.
Sometimes other procedures are needed at the same time and these may impact the recovery protocol. It is important to have a skilled physical therapist to ensure the optimal result.
DFO procedures are challenging, and reported complicated rates range from 5% to 63%5. If screws are placed too close to the joint, patients can suffer from intra-articular fractures. Screw and plate failure can occur as well as malunion. If patients are too active too quickly, they can suffer implant failure and collapse of the osteotomy site. Other complications include but are not limited to a pulmonary embolism, anterior knee pain, and arthrofibrosis.
Dr. Gilmer’s Take:
The DFO is a powerful procedure that treats the most common deformity resulting in a valgus ‘knock kneed’ stance.
Most of my patients have had prior meniscus surgery, often meniscectomy where some or all of the meniscus has been removed, or ACL surgery which can lead to injury to the cartilage in the outer part of the knee. In other cases, these patients just have wear and tear from being out of alignment. I have found that many times, the osteotomy is the most important part of preserving these knees and that this is more important than the most intuitive procedures such as replacing the cartilage (OCA, OATS surgeries) or meniscal transplant. After a successful osteotomy patients have no restrictions and can even do higher impact activities.
The two most common issues I see with the DFO are the need to remove the large plate, especially common in smaller patients, and the fact that for geometric reasons, the DFO only corrects the alignment when the knee is near extension. This means it may not be as helpful in protecting the knee cartilage when the knee is flexed more. Correction on the tibia by comparison, corrects the deformity in both flexion and extension. This concept is also important in total knee replacement and partial knee replacement.
In my practice DFO is typically for younger patients where joint replacement (arthroplasty) is not a good option because of the risk of premature wear of the metal and plastic components or patients who want to have higher impact activities which are not recommended with joint replacement.
Brian Gilmer, August 2023
Citations
- Song SK, Choi WK, Jung SH, Kim HC, Kim TH, Cho MR. Changes of acetabular anteversion according to pelvic tilt on sagittal plane under various acetabular inclinations. J Orthop Res. 2021 Apr;39(4):806-812. doi: 10.1002/jor.24790. Epub 2020 Jul 10. PMID: 32603527.
- Bhaskar D, Rajpura A, Board T. Current Concepts in Acetabular Positioning in Total Hip Arthroplasty. Indian J Orthop. 2017 Jul-Aug;51(4):386-396. doi: 10.4103/ortho.IJOrtho_144_17. PMID: 28790467; PMCID: PMC5525519.
- Rosso F, Margheritini F. Distal femoral osteotomy. Curr Rev Musculoskelet Med. 2014 Dec;7(4):302-11. doi: 10.1007/s12178-014-9233-z. PMID: 25142271; PMCID: PMC4596223.
- Sabbag OD, Woodmass JM, Wu IT, Krych AJ, Stuart MJ. Medial Closing-Wedge Distal Femoral Osteotomy with Medial Patellofemoral Ligament Imbrication for Genu Valgum with Lateral Patellar Instability. Arthrosc Tech. 2017 Nov 6;6(6):e2085-e2091. doi: 10.1016/j.eats.2017.08.012. PMID: 29349001; PMCID: PMC5766318.
- Nakamura R, Akiyama T, Takeuchi R, Nakayama H, Kondo E. Medial Closed Wedge Distal Femoral Osteotomy Using a Novel Plate With an Optimal Compression System. Arthrosc Tech. 2021 May 7;10(6):e1497-e1504. doi: 10.1016/j.eats.2021.02.016. PMID: 34258196; PMCID: PMC8252853.
- Chahla, Jorge, et al. "Opening-and closing-wedge distal femoral osteotomy: a systematic review of outcomes for isolated lateral compartment osteoarthritis." Orthopaedic Journal of Sports Medicine 4.6 (2016): 2325967116649901.
- Healy, W. L., et al. "Distal femoral varus osteotomy." JBJS70.1 (1988): 102-109.
- O'Malley, Michael P., et al. "Distal femoral osteotomy: lateral opening wedge technique." Arthroscopy Techniques 5.4 (2016): e725-e730.
- Sabbag, Orlando D., et al. "Medial closing-wedge distal femoral osteotomy with medial patellofemoral ligament imbrication for genu valgum with lateral patellar instability."Arthroscopy techniques 6.6 (2017): e2085-e2091.
- 10. Sharma, Leena, et al. "The role of knee alignment in disease progression and functional decline in knee osteoarthritis." Jama 286.2 (2001): 188-195.
- Thein, Rafael, et al. "Distal femoral osteotomy for valgus arthritic knees." Journal of orthopaedic science 17.6 (2012): 745-749.
Max Whooley is a first-year medical student attending Creighton University School of Medicine in Phoenix, Arizona.
Kayla Aikins is currently a third year medical student at the University of Nevada, Reno School of Medicine.










