Zoe Anderson MS2, Brian Gilmer, MD
Introduction
High tibial osteotomy (HTO) is a surgical procedure that can improve joint alignment and contribute to joint preservation. HTO entails osteotomy (cutting of bone) in the tibia to realign the knee joint. HTO results in decreased load on damaged joints, delaying osteoarthritis.2 HTO can preserve the joints and delay the need for total knee replacement.
This term can be a little misleading as the tibia can be cut to correct a varus (bow-legged) deformity or a valgus (knock-kneed) deformity. In practice and for the purposes of this article we are referring to cutting the tibia bone to correct a varus deformity (bow legged) for patients with medial compartment (inside of the knee) problems. This is in part because it is more common for the deformity to be located in the tibia bone, and in general, we try to correct the deformity in the bone that it occurs in – varus usually in the tibia and valgus usually in the femur.
Indications
HTO is not particularly common in the United States, but is more common in Europe and Asia. It is generally used for young, active patients2, as it can delay the need for knee replacement surgery.1 Furthermore, knee replacement or even partial knee replacement has limitations in some patients who want to return to higher impact activities. Knee replacements wear out faster than native joints do. Also, younger patients might need a second or third knee replacement over their lifetimes and in general these revision knee replacements do not have quite the same outcomes as the first knee replacement. Hence it is best to delay knee replacement when possible.
While each case is unique, the usual candidate for HTO is a patient under 60 with isolated medial osteoarthritis (inside part of knee), good range of motion, and with no ligamentous instability.3 HTO may also be indicated in young, active patients who present with varus knees and symptoms of medial compartment arthritis.4 Sometimes this occurs because patients have had prior trauma or surgery such as meniscectomy or have had cartilage injury.
Skilled surgeons have expanded the inclusion criteria for HTO, and these osteotomies are now sometimes performed in patients under 40 and in overweight patients.5 Guidelines indicating HTO are a patient with isolated medial joint line pain, aged 40 to 60, BMI<30, high-demand activity including running or jumping, malalignment <15 degrees, metaphyseal varus (the deformity is in the tibia thing again), full range of movement, and normal lateral and patellofemoral compartments (the other parts of the knee, outside and under the knee cap).6
Causes
Osteoarthritis of the knee is the result of wear and tear commonly due to aging, resulting in the loss of cartilage. Primary osteoarthritis of the knee is caused by articular degeneration in the absence of an underlying issue. Secondary osteoarthritis of the knee is caused by an underlying issue, fracture, meniscal tears, ACL tears, all of which can lead to abnormal distribution of forces across the joint or trauma.7
Imagine that one of the tires on your car was not in proper alignment and one edge of the tire was on the road while the other side of the tire was not. This would lead one side of the tire to wear out faster.
 Figure 1 showing the uneven malaligned tire analogy
Figure 1 showing the uneven malaligned tire analogy
This shows a similar process in the knee. The knee on the left hand side of the picture has less space between the bones on the inside. This indicates more pressure on the medial side of the knee has led to wear of the cartilage. This patient was only 35 years old at the time of the x-ray. The knee on the right has more or less equal amount of space in both parts of the knee. Space on xrays taken when the patient is standing up show how much cartilage is left because cartilage does not appear on xrays but if it is there, it will hold the bones apart. Normal knee joints have around 4mm of cartilage space between the bones
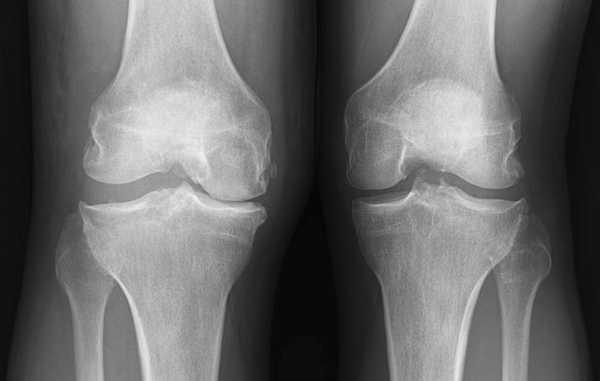 Figure 2
Figure 2
Diagnosis
A surgeon or orthopedic specialist can diagnose medial compartment osteoarthritis based on medical history, physical exam, and imaging, such as radiography and MRI.
In addition to standing xrays like the one shown above a full length x-ray is taken which shows the alignment of all the bones in the leg, tibia and femur, and allows the surgeon to determine where the weight bearing axis is. That is the line from the hip down to the ankle that shows where most of the weight in the leg crosses the knee joint. If this line crosses through the inside of the knee joint, the deformity is varus. If through the outside, the deformity is called valgus.
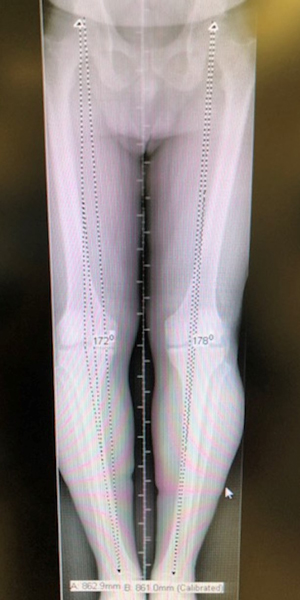 Figure 3
Figure 3
In this standing alignment film the leg on the left side of the image has much more varus deformity. You can see how this person would appear bow legged when seen in the office standing up. This patient ultimately underwent an osteotomy to correct the deformity.
Procedure
Numerous HTO approaches exist, with opening wedge HTO being the most commonly performed.3 This is true in Dr. Gilmer’s practice as well.
Medial opening wedge osteotomy consists of a single osteotomy. A vertical incision is made between the medial aspect of the tibial tuberosity and the posteromedial aspect of the tibia beneath the joint line.3 A cut is made in the tibia, and the surgeon indicates the size of the intended wedge using guide wires. Next, the surgeon will cut at an angle along the guide wires, removing the wedge of bone, and inserting a bone graft that fills the space, leaving the wedge open.9
The specific technique that Dr. Gilmer typically uses can be seen here in an animation
In some cases a plate is used to hold the gap open. This can be used when a correction of the tibial slope is performed at the same time or when the correction is large or for larger patients. Many times this plate will need to be removed. When possible the lower profile plastic implant is used to reduce the need for hardware removal later.
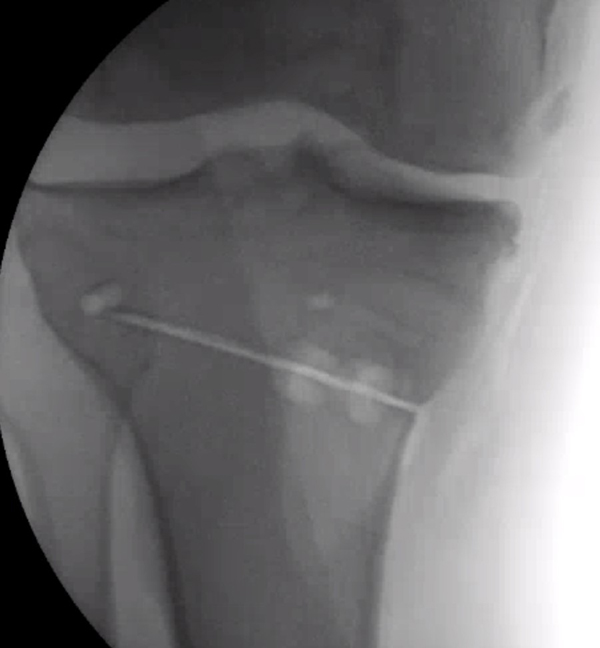 Figure 4
Figure 4
First a hole is drilled and a single cut is made in the tibia bone. The surgeon must be very careful to protect the nerves and arteries behind the leg.
Then a jack is inserted to slowly and carefully separate the bone edges. In this image the line running from top to bottom is running from the hip to the ankle to show how the weight bearing axis is being corrected as the osteotomy is slowly opened.
Finally, the plastic wedge and screws are inserted. The small dark lines are metal markers inserted in the plastic so that the surgeon can see the implant on xray since plastic does not show up on x-rays.
Though less common, in a closing wedge osteotomy, bone is removed from the tibia, and the gap is closed by fastening the edges together.1 This technique involves an osteotomy above the tibial tubercle and the removal of a wedge of bone laterally.10
Post-Operative Care
For medial opening wedge osteotomy, joint exercises should be initiated early on, and partial weight bearing exercises should be performed with the knee in a hinged brace for 6 weeks.3 Weight bearing can progressively be increased between 6 and 12 weeks.3 Routine radiography may be performed to assess alignment.
For lateral closing wedge osteotomy, partial weight bearing exercises are allowed immediately post-operatively. A hinged knee brace should be worn for 6 weeks and weight bearing can be progressively increased.
Risks and Complications
As with any knee surgery, possible risks include knee stiffness, infection, blood clots, nerve and blood vessel damage, and ligament injuries.8 Compartment syndrome, fractures, pseudoarthrosis, and nonunion are other potential complications.3,10
Dr. Gilmer’s Take
Much like the distal femoral osteotomy. The HTO is a powerful procedure that treats the most common deformity resulting in a varus bow legged stance.
Most of my osteotomy patients have had prior surgery, often meniscectomy where some or all of the meniscus has been removed, or ACL surgery which can lead to injury to the cartilage in the inner part of the knee. In other cases, these patients just have wear and tear from being out of alignment. I have found that many times, the osteotomy is the most important part of preserving these knees and that this is more important than the most intuitive procedures such as replacing the cartilage (OCA, OATS surgeries) or meniscal transplant. After a successful osteotomy patients have no restrictions and can even do higher impact activities.
The two most common issues I see with the HTO are the need to remove the large plate, and thus I have taken to using a plastic (PEEK) implant when possible. The other risk is a hinge fracture where the small hinge point of the osteotomy cracks out. This can require additional surgery and I try very hard to avoid this at all costs.
In my practice HTO is typically for younger patients where joint replacement (arthroplasty) is not a good option because of the risk of premature wear of the metal and plastic components or patients who want to have higher impact activities which are not recommended with joint replacement.
Brian Gilmer, MD – February 2023
References
- High tibial osteotomy knee surgery and realignment: HSS. Hospital for Special Surgery. (2018, October 16). Retrieved December 28, 2022, from www.hss.edu/conditions_knee-surgery-high-tibial-osteotomy.asp
- Sabzevari, S., Ebrahimpour, A., Roudi, M. K., & Kachooei, A. R. (2016). High tibial osteotomy: a systematic review and current concept. Archives of Bone and Joint Surgery, 4(3), 204.
- Lee, D. C., & Byun, S. J. (2012). High tibial osteotomy. Knee surgery & related research, 24(2), 61.
- Elson, D. W., Paweleck, J. E., Shields, D. W., Dawson, M. J., & Ferrier, G. M. (2013). Stretching the indications: high tibial osteotomy used successfully to treat isolated ankle symptoms. Case Reports, 2013, bcr2013200527.
- Seil, R., van Heerwaarden, R., Lobenhoffer, P., & Kohn, D. (2013). The rapid evolution of knee osteotomies. Knee Surgery, Sports Traumatology, Arthroscopy, 21(1), 1-2.
- Gao, L., Madry, H., Chugaev, D. V., Denti, M., Frolov, A., Burtsev, M., Magnitskaya, N., Mukhanov, V., Neyret, P., Solomin, L. N., Sorokin, E., Staubli, A. E., Stone, K. R., Vilenskiy, V., Zayats, V., Pape, D., & Korolev, A. (2019). Advances in modern osteotomies around the knee : Report on the Association of Sports Traumatology, Arthroscopy, Orthopaedic surgery, Rehabilitation (ASTAOR) Moscow International Osteotomy Congress 2017. Journal of experimental orthopaedics, 6(1), 9. www.doi.org/10.1186/s40634-019-0177-5
- Hsu, H., & Siwiec, R. M. (2018). Knee osteoarthritis.
- (n.d.). Total knee replacement (TKR). Total Knee Replacement Mammoth Lakes, CA. Knee Osteoarthritis CA. Retrieved December 28, 2022, from www.mammothortho.com/total-knee-replacement-mammoth-orthopedic-institute.html
- Open wedge tibial osteotomy. AOA Orthopedic Specialists. (2021, August 6). Retrieved December 28, 2022, from www.arlingtonortho.com/conditions/knee/knee-tibial-osteotomy-with-open-wedge/
- Tunggal, J. A., Higgins, G. A., & Waddell, J. P. (2010). Complications of closing wedge high tibial osteotomy. International orthopaedics, 34(2), 255–261. https://doi.org/10.1007/s00264-009-0819-9
Biography: Zoe Anderson is currently a second-year medical student at the University of Nevada, Reno School of Medicine.










