
MCL Reconstruction Surgeon in Reno, NV
A direct impact to the knee can cause an injury to the medial collateral ligament (MCL) leading to minor sprain and pain, swelling, a partial or complete tear of the ligament or joint instability. Dr. Gilmer provides diagnosis and minimally-invasive MCL reconstruction surgery in Reno, NV. Dr. Gilmer also provides highly specialized care during and after the surgery. Contact Dr. Gilmer’s office for an appointment today!
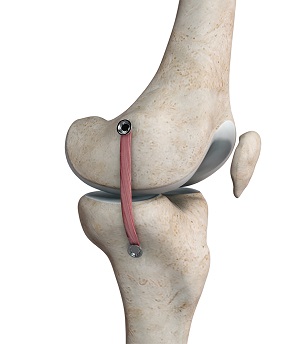
Medial Collateral Ligament – Encyclokneedia
Introduction:
The Median Collateral Ligament (MCL) is a strong band of tissue that runs along the inner aspect of the knee joint, and its primary function is to provide stability to the knee by resisting valgus forces. Excess valgus force or significant twisting of the lower extremity can injure this ligament, with patients often complaining of medial knee pain, swelling, and may or may not experience joint instability when ambulating.
MCL injuries are relatively common, especially among athletes who participate in contact sports such as football and soccer, as well as those which require significant twisting and torque of the lower extremities like skiing. It’s estimated that ligament injuries account for 40% of all knee injuries, and of those, MCL injuries were the most common [1]. Isolated MCL injuries are uncommon as other structures of the knee are often damaged in conjunction with the MCL due to its intimate relationship with other structures in the knee, however the rate of isolated MCL injuries tends to vary depending on the mechanism of injury.
Anatomy:
The knee joint is composed of the distal femur and proximal tibia and fibula, connected by a capsule, with numerous soft tissue structures overlying and surrounding the joint which provide support and stability. These soft tissue structures are tightly packed together and thus can be hard to distinguish from one another. Due to this, these structures are grouped together and make up the capsuloligamentous complex of the knee. This complex consists of both static and dynamic structures, with the dynamic stabilizers including the vastus medialis, semimembranosus, gracilis, and sartorius muscles. The static stabilizers, which are relatively complex and intertwined with one another can be divided into three layers. From superficial to deep they are as follows [11][12]:
- Deep sartorial fascia
- Superficial MCL, posterior oblique ligament, oblique popliteal ligament, posterior horn of the medial meniscus
- Deep MCL, posterior medial capsule.
The MCL itself is an 8-10 cm long, thin, hourglass shaped ligament that originates from the medial femoral condyle and inserts into the anterior medial tibia. The deep MCL, along with the posterior oblique ligament is attached to the medial meniscus and thus moderate to severe MCL injuries may also involve the medial meniscus [9]. Vascularization to the MCL is supplied via the genicular arteries which arise from the popliteal artery. Innervation is supplied by the medial articular nerve which arises off the saphenous nerve. Other clinically significant structures of the medial knee include the medial gastrocnemius tendon, medial hamstring tendon, adductor magnus tendon and the medial patella-femoral ligament [13].
History:
MCL injuries are classified in grades 1-3 depending on the severity of injury. Grading can be accomplished through MRI of the knee to visualize the MCL or through physical exam maneuvers by looking for joint opening when applying a valgus stress to the knee. Of note, the grading system is known to be somewhat inconsistent in its clinical correlation to severity and instability of injury. Grades are as follows:
- - Grade 1: MRI imaging shows no tearing of the MCL. Physical exam demonstrates 5 mm of joint opening with a solid endpoint. Damage is limited to a sprain of the ligament.
- - Grade 2 = MRI imaging shows a partial tear. Physical exam testing reveals 5-9 mm of joint opening with a clear endpoint usually present.
- - Grade 3 = MRI imaging shows a complete tear, physical exam testing will reveal 10 mm or more of joint opening with no clearly defined endpoint.
MCL injuries are the result of a valgus force applied through the knee, often with concurrent tibial rotation or knee hyperextension. This can be accomplished through a direct means where a strong valgus force is applied through the knee, often secondary to physical contact such as a tackle. Injury may also be sustained indirectly from lower extremity abduction or tibial rotation, indirectly generating similar valgus forces on the MCL as seen in direct injuries. Direct injuries are thought to be more common than those from an indirect mechanism, with a study performed by Lundblad in 2013 finding that 75% of MCL injuries sustained by members of the Union of European Football Association were from a direct mechanism. Injuries from direct contact also tend to be more severe than non-contact injury [3][6].
Indirect injury is more often the result of a strong cutting or pivoting movement while at speed, seen in sports such as skiing, tennis, and soccer. When the foot is planted or becomes caught on the ground while attempting to change direction, lower extremity abduction and tibial rotation occur which generates a similar net force to that of a direct contact injury. Additionally, if the knee is hyperextended at the time of injury, the peroneal nerve may also be at risk of sustaining damage as is seen more commonly in lateral knee injuries [14].
Due to the high forces required to injure the MCL, this is an injury typically seen in those participating in athletics. The risk of injury varies among individuals based upon a variety of factors such as the chosen sport as well as the biomechanics unique to each person. Sports with the greatest risk of injury were those which involve direct physical contact such as wrestling, hockey, and American football, along with sports which require quick movements while at speed such as soccer and basketball. Other risk factors include prior knee injury, competition events (as opposed to practice events – presumably due to an increased willingness to take risk) and a higher level of play (i.e., performing at the collegiate level vs high school) [4]. Sex has also been postulated to serve as a potential risk factor, however studies have been unable to come to a conclusive decision on the exact role it may play. Some studies have found that females are at an increased risk of sustaining an MCL injury at the high school and collegiate levels, whereas other studies showed the risk of injury was higher among male collegiate athletes, however risk was still greater for females at the high school level [4][5][7].
Isolated MCL injury is relatively uncommon due to the high force necessary to sustain injury in conjunction with the numerous ligamentous attachments throughout the knee. Medial meniscus tears are estimated to occur in 5% of MCL injuries, and injury to other ligaments has been found to occur in 20 – 78% of cases, depending on severity and mechanism of injury [8]. In grade 3 injuries, approximately 78% of cases involved trauma to multiple ligaments and of these cases, the ACL was injured in 95% of them [9][10].
Physical Exam:
Examination of the knee after suspected MCL injury is best performed within 20-30 minutes of when the initial injury was sustained. This is because the patient and knee must be relaxed for complete evaluation, and this time period is ideal as pain and swelling are unlikely to have progressed enough to prevent examination. Unfortunately, examination within this time frame is not always possible, especially outside of major sporting events where healthcare professionals are not readily available on standby.
Examination should start with careful inspection of the entire patient, looking for changes or instability of the patient’s gait and resting stance. Inability to bear weight on the injured leg is indicative of a severe injury and further workup should be pursued immediately. Inspection should then be focused on the knee, looking for erythema, ecchymosis, and signs of deformities or fractures. Swelling may or may not be present depending on the severity of injury, and in traumatic cases may be secondary to a joint effusion.
Following inspection, the examiner should move on to palpation of the knee. Begin by palpating the full length of the MCL, noting any tenderness along the way as this may indicate where the injury was sustained [8]. Bony landmarks such as the tibial tubercle, tibial metaphysis, tibial plateau, posterior medial corner, posterior and lateral femoral condyles, patella and facets, and joint lines should also be palpated. Tenderness along the medial joint line can be indicative of a mid-substance tear, however medial meniscus injury should be ruled out before final diagnosis [8]. Additionally, the soft tissues of the capsuloligamentous complex of the knee - including the stabilizing muscles - should be palpated to inspect for concomitant injuries.
Range of motion testing is critical in these cases to assess severity of injury. The examiners should start by evaluating the uninjured knee to establish base line mobility, and then proceed to the injured knee, comparing mobility limits to the normal knee. Active, passive and resisted range of motion should be tested, however passive testing is not necessary if there is full and unrestricted mobility on active testing. On resisted motion testing, inability to complete a straight leg raise should raise concern for a joint effusion and thus further imaging is warranted.
Valgus stress testing at 0 and 30 degrees of knee flexion is imperative to help establish a grade of injury when suspecting an MCL injury. This is completed by having the patient lie in the supine position, with their hip slightly flexed and leg slightly abducted. Have the patient bend their knee to the specified angle (30 or 0 degrees). The examiner may then apply a valgus force through the knee, looking for joint opening, laxity, and endpoints. Positive findings at 30 degrees of flexion are indicative of injury to the superficial MCL while positive findings at 0 degrees is likely due to deep MCL injury and may also involve a cruciate ligament as these ligaments act as secondary resistors of valgus stress. Tibial rotation may also be measured by rotating the foot while simultaneously palpating the joint line. Rotational instability witnessed on exam should raise concern for injury to the deep MCL [26].
Imaging:
When discussing imaging of soft tissues of the body, MRI is thought of as the gold standard. Despite this, it is rarely deemed necessary to evaluate low grade MCL injuries. Rather, MRI’s primary use is in defining the extent of severe injuries and to look for other injuries or structural changes in the knee [17]. It serves a significant role in evaluation of grade 3 injuries and may be able to further specify whether the injury occurred to the deep or superficial MCL and may be able to indicate the location of the tear [19]. It can also have significant use in patients who are skeletally immature and hold a greater risk for an avulsion fracture in knee injuries, as these are likely to go unnoticed on alternative imaging studies which may impair recovery [20]. MRI can aid in determining the grade of injury; however, the current grading scheme is known to be somewhat inconsistent in its correlation to the clinical severity of the injury along with the instability of the joint [17][18]. A wide variety of imaging findings are seen in MCL injuries, and broadly include soft tissue swelling, ligament tears, contusions, meniscal injury, hemarthroses, bursitis, and ligamentous injury [8].
While radiographs are unable to visualize soft tissue structures, they do prove to be useful in settings where a patient is unable to bear weight on the injured extremity, has bony tenderness or deformities, or if there is a suspected joint effusion. When indicated, radiographs of the AP, lateral, and patellar views should be obtained [16] for further evaluation.
Ultrasound is becoming more commonplace thanks to its being a fast, cheap, and safe means of imaging. MCL lesions may be identified on ultrasound via their abnormal echogenicity leading to an altered appearance. While not as useful in the setting of traumatic and multiligamentous injuries, when suspecting an isolated MCL injury, ultrasonography may be the preferred imaging method due to its high spatial resolution and ability to immediately compare findings to the contralateral knee [21].
Treatment:
Treatment of and recovery from an MCL injury is primarily accomplished by starting with basic care and progressing to rehabilitation. Initial treatment begins with evaluation by the appropriate medical professional. Your primary care provider or an emergency medicine physician may be able to assess the injury and guide treatment. In more severe injuries, orthopedic referral may be indicated. Surgical repair and casting were previously the standard treatment option, however numerous observational studies have shown the effectiveness and decreased morbidity of bracing and physical rehabilitation when compared to surgical repair of isolated MCL injuries [2]. Thus, surgical treatment is only indicated for patients with severe and concomitant injuries. Referral to an orthopedic surgeon should be sought for:
- Knee instability
- Displaced fractures, Angulated fractures
- Injuries that involve the physis
- Injuries of the distal MCL
- Injuries involving structures of the posteromedial corner or ACL
- Injuries in which pain persists for multiple weeks following initial insult
As mentioned prior, Isolated MCL injuries are somewhat uncommon, and while patients may anticipate a non-operative recovery from an such an injury, damage to other soft tissue structures may complicate treatment and recovery.
Following evaluation, treatment starts with basic interventions consisting of the RICE method, analgesics for pain, and knee bracing (traditionally a hinge brace to help stabilize the knee, prevent valgus forces from causing further injury, and preventing complete extension of the knee.) Studies have shown that immobilizing the joint is associated with worse patient outcomes [15]. Rather, observational data has shown that early motion is associated with strong ligament healing and tensile strength. Thus, in early treatment the goal is regain function and mobility of joint while continuing to protect and support it to prevent further injury [3]. This may be accomplished via exercises which specifically strengthen the MCL in combination with general activity movements starting with walking and progressing up to jogging, sprinting, and finally rapid movement and sports specific drills. Patients often return to sport quickly and safely, and the timing of the decision to return is made upon individual progress. Upon regaining full active range of motion, strength, and ability to perform necessary activities and movements demanded by the sport, patients may return. General estimates place the window of recovery between three and six weeks.
Dr. Gilmer’s Take
MCL injuries have always been a common area of research and clinic interest for me, in part, because they are pretty common in skiers, especially when combined with ACL injury. In 2023, I addressed this in an editorial in the Arthroscopy Journal that can be found here.
My preferred technique evolved from reviewing older techniques and doing allograft reconstruction cases where the fixation on the tibia was very near the insertion of the pes anserine tendons. As a result, I gradually moved to harvesting the semitendinosus tendons and leaving it attached to the tibia. This technique is familiar since it is the same (almost) as harvesting for a hamstring ACL reconstruction. The tendon is then redirected to just 1cm-2cm below the medial joint line where it can be fixed with suture anchors or a button and tightrope that traverses the proximal tibia (a trick learned from Dr. Hatch at USC). The isometric point is then found on the femur and the tendon is fixed there with a loop on a second tightrope. This recreates a short construct that is a modification of the Bosworth technique. I described this technique with my mentor Dr. Chris Wahl and it can be found published here.
The change I have made since 2022 with this technique is from using screw fixation on the femur to a button fixation that allows for retensioning after the knee is cycled and I have found to have more robust fixation without risk of slippage of the graft or the screw. This short construct idea was recently validated in a biomechanical study in AJSM-
This makes sense because the working length of the graft is shorter and also it is less morbid for the patient, meaning less dissection and a shorter incision. The other change is simply being more certain to run the graft directly against the bone. Particularly, when there is a chronic injury there is often a thick scar and this can keep the graft from working optimally against the surface of the femur. I think some cases of laxity can be attributed to this as I have seen the graft laying over a dense and thickened scar of the MCL
No doubt, this area will continue to evolve. My general approach to timing is to wait about 4 weeks in cases where healing seems reasonably likely and then reevaluate, if there is some healing, you can proceed with ACL surgery and trust that healing will continue. This is often the time needed for obtaining baseline prehab motion and balances against a longer delay. Ultimately, the final decision is made intraoperatively by evaluating the gapping of the compartment during the diagnostic arthroscopy and I counsel patients that this may alter the rehab a bit as we generally protect MCL reconstructions for 4 weeks of protected weight bearing followed by gradual 2 week crutch wean which is more restrictive than the ACL protocol alone.
Brian Gilmer, May 2024
Citations:
- Posch M, Schranz A, Lener M, Tecklenburg K, Burtscher M, Ruedl G. In recreational alpine skiing, the ACL is predominantly injured in all knee injuries needing hospitalisation. Knee Surg Sports Traumatol Arthrosc. 2021;29(6):1790-1796.
- Wilk KE, Andrews JR, Clancy WG. Nonoperative and postoperative rehabilitation of the collateral ligaments of the knee. Operative Techniques in Sports Medicine. 1996;4(3):192-201.
- Lundblad M, Waldén M, Magnusson H, Karlsson J, Ekstrand J. The UEFA injury study: 11-year data concerning 346 MCL injuries and time to return to play. Br J Sports Med. 2013;47(12):759-762.
- Roach CJ, Haley CA, Cameron KL, Pallis M, Svoboda SJ, Owens BD. The epidemiology of medial collateral ligament sprains in young athletes. Am J Sports Med. 2014;42(5):1103-1109.
- Swenson DM, Collins CL, Best TM, Flanigan DC, Fields SK, Comstock RD. Epidemiology of knee injuries among U.S. high school athletes, 2005/2006-2010/2011. Med Sci Sports Exerc. 2013;45(3):462-469.
- Lundblad M, Hägglund M, Thomeé C, et al. Medial collateral ligament injuries of the knee in male professional football players: a prospective three-season study of 130 cases from the UEFA Elite Club Injury Study. Knee Surg Sports Traumatol Arthrosc. 2019;27(11):3692-3698.
- Stanley LE, Kerr ZY, Dompier TP, Padua DA. Sex Differences in the Incidence of Anterior Cruciate Ligament, Medial Collateral Ligament, and Meniscal Injuries in Collegiate and High School Sports: 2009-2010 Through 2013-2014. Am J Sports Med. 2016;44(6):1565-1572.
- Singhal M, Patel J, Johnson D. Medial ligament injuries. In: DeLee and Drez Orthopaedic Sports Medicine, DeLee J, Drez D, Miller M (Eds), Saunders, Philadelphia 2010. p.1629.
- Fetto JF, Marshall JL. Medial collateral ligament injuries of the knee: a rationale for treatment. Clin Orthop Relat Res. 1978;(132):206-218.
- Grant JA, Tannenbaum E, Miller BS, Bedi A. Treatment of combined complete tears of the anterior cruciate and medial collateral ligaments. Arthroscopy. 2012;28(1):110-122.
- Warren LF, Marshall JL. The supporting structures and layers on the medial side of the knee: an anatomical analysis. J Bone Joint Surg Am. 1979;61(1):56-62.
- Fanelli GC, Harris JD. Surgical treatment of acute medial collateral ligament and posteromedial corner injuries of the knee. Sports Med Arthrosc Rev. 2006;14(2):78-83.
- LaPrade RF, Moulton SG, Nitri M, Mueller W, Engebretsen L. Clinically relevant anatomy and what anatomic reconstruction means. Knee Surg Sports Traumatol Arthrosc. 2015;23(10):2950-2959.
- Takagi T, Nakao Y, Takayama S, Toyama Y. Traction injury of common peroneal nerve associated with multiple ligamentous rupture of the knee: a case report. Microsurgery. 2002;22(8):339-342.
- Creighton RA, Spang JT, Dahners LE. Basic Science of Ligament Healing. Sports Medicine and Arthroscopy Review. 2005;13(3):145-150.
- Kurzweil PR, Kelley ST. Physical examination and imaging of the medial collateral ligament and posteromedial corner of the knee. Sports Med Arthrosc Rev. 2006;14(2):67-73.
- Meyer P, Reiter A, Akoto R, et al. Imaging of the medial collateral ligament of the knee: a systematic review. Arch Orthop Trauma Surg. 2022;142(12):3721-3736.
- Schein A, Matcuk G, Patel D, et al. Structure and function, injury, pathology, and treatment of the medial collateral ligament of the knee. Emerg Radiol. 2012;19(6):489-498.
- Nakamura N, Horibe S, Toritsuka Y, Mitsuoka T, Yoshikawa H, Shino K. Acute grade III medial collateral ligament injury of the knee associated with anterior cruciate ligament tear. The usefulness of magnetic resonance imaging in determining a treatment regimen. Am J Sports Med. 2003;31(2):261-267.
- Jarrett DY, Kramer DE, Laor T. Magnetic resonance imaging of medial collateral ligament avulsion fractures of the knee in children: a potentially underestimated injury [published correction appears in Pediatr Radiol. 2021 May 29;:]. Pediatr Radiol. 2021;51(9):1705-1713.
- Alves TI, Girish G, Kalume Brigido M, Jacobson JA. US of the Knee: Scanning Techniques, Pitfalls, and Pathologic Conditions. Radiographics. 2016;36(6):1759-1775.
If you would like to have additional information on the treatment of MCL injury or would like to learn more about MCL reconstruction, please contact Dr. Gilmer, serving the communities of Reno, NV.










